Hey there,
It’s Mikal Khoso and welcome to Trajectory, a newsletter about where the world is heading, delivered straight to your inbox.
The High-Level This Week
There is a quiet public health crisis brewing globally. Diseases of autoimmunity are soaring globally and 23.5m Americans live with an autoimmune disease.
Autoimmune diseases are diseases where the immune system attacks health cells such as hair, stomach, pancreatic and other cells. Examples of Autoimmune diseases are Type 1 Diabetes, Multiple Sclerosis and Hashimoto’s Disease.
Incidences are significantly higher in the developed world versus the developing. Research has shown migrants from Asia (low incidence of autoimmune diseases) to the US or Europe (high incidences) see their children develop high incidences of autoimmune diseases.
The rise of autoimmune diseases has been theorized as linked to the decreasing diversity of our microbiome thanks to chemical exposure and lifestyle changes.
To learn more, read on.
If you haven’t already, subscribe here. If you liked this week’s edition and think someone else you know would find it interesting please take a couple seconds to share it via email or on social media.
Intellectual Sparks
American business schools are reinventing the MBA: A new future for the MBA?
Exclusive: U.S. opens national security investigation into TikTok: Chinese Social media app Tik Tok is under investigation by the US Government for data privacy concerns.
The United States Should Fear a Faltering China: China despite all its growth is at a vulnerable moment and likely to lash out politically and militarily as a result.
The Asian century is set to begin: Nonetheless the Asian century is about to begin.
How to Stop the Abuse of Location Data: In an Op-ed Foursquare CEO lends his insight on the subject.
Key Issue: The Autoimmunity Crisis
Across the world a health crisis is quietly brewing. Diseases of autoimmunity are soaring across the globe and particularly so in the developed world. An autoimmune disease is when otherwise healthy cells provoke an immune response and are attacked and destroyed by the immune system. Autoimmune diseases are particularly pernicious because they attack the body from the inside out and use its own defenses against itself.
For a long time, autoimmune diseases hid in plain sight. Diseases such as diabetes and inflammatory bowel syndrome were treated as completely independent and unrelated. It wasn’t till the scientific community noticed a common thread among a large category of diseases – the immune response. Today, over 100 diseases have been identified and classified as part of the autoimmune family of diseases. They range broadly in scope and severity:
Rheumatoid arthritis: immune system attacks joints
Alopecia areata: immune system attacks hair follicles, causing hair loss
Type 1 Diabetes: Immune system attacks pancreas and cells that produce insulin
Lupus: Immune system attacks various tissues within body
Multiple Sclerosis: Immune system attacks nerve cells
Inflammatory Bowel Disease: Immune system attacks lining of intestinesHashimoto’s disease: Immune system attacks thyroid glands
Autoimmune diseases come in two varieties: organ specific and systemic varieties. Type 1 Diabetes for example is an organ-specific disease while Multiple Sclerosis is a systemic one.
Diseases of autoimmunity are rapidly becoming an epidemic especially so in the developed world. The National Institute of Health (NIH) in the United States reports that 23.5 million Americans live with an autoimmune condition. The American Autoimmune Related Diseases Association (AARDA) estimates that number is closer to 50 million Americans, citing incomplete data. In the United Kingdom 4 million people live with an autoimmune condition, nearly 10% of the population.
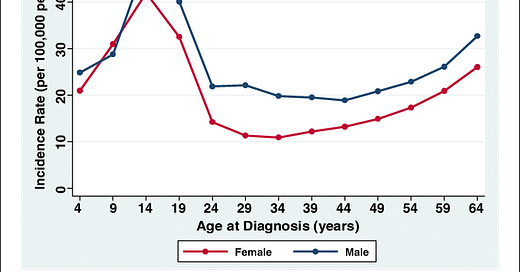
Incidence rates for type 1 diabetes by age at diagnosis and sex, United States, 2001-2015

Worryingly incidences of autoimmune conditions are rising rapidly across the world. Today 1.25 million people live with Type 1 Diabetes in the United States. But this is rising and most rapidly in children. A recent study from the Center for Disease Control and Prevention found that between 2002 and 2012 the rate of new diagnosed cases of type 1 diabetes in youth increased by about 1.8 percent each year.
The Causes of Autoimmunity Diseases
Genetic Causes
Our understanding of the causes of autoimmune conditions is limited. Scientists have theorized everything from genetics, chemical exposure and changes to our gut bacteria as causes for the conditions. The limited research so far makes it clear that genetics plays some role. Autoimmune conditions have been found to cluster in families and if one member of a family has an autoimmune condition, other members are more likely to develop a condition as well.
But genetics plays a poor predictive and explanatory role in analyzing the rise of autoimmune conditions. For example, studies have found that the incidence of diabetes is sixfold higher in Finland compared to the adjacent Karelian republic of Russia, although the genetic background is the same.
Chemical Exposure and Environmental Causes
Chemical exposure and environmental conditions have also been offered as possible triggers for autoimmune conditions. This would help explain the incidence differences between Finaland and the Karelian Republic. Incredibly, studies focused on migration patterns have shown that subjects migrating from countries with a low-incidence of autoimmune diseases to high-incidence countries acquire the immune disorders with a high incidence at the first generation. This has been illustrated across populations and regions. For example, a study found an increasing frequency of diabetes in families of immigrants from Pakistan to the United Kingdom. A similar study also found an increasing risk of multiple sclerosis in Asian immigrants moving to the United States. Finally, research has shown that the prevalence of systemic lupus erythematosus (SLE) is also much higher in African Americans compared to West Africans.
Chemical contamination is a chronic issue across the world. Recently, Per- and polyfluoroalkyl substances (PFAS) have been the focus of much attention globally. PFAS exposure can cause low infant birth weights, immune effects, cancer, thyroid disruption and more and can be found in food, the water supply, household products and living organisms (like cattle). This map shows the number and range of PFAS contaminated sites across the United States.

PFAS contaminated sites in the Northeast United States. Source.
A 2003 study found 210 chemicals in Americans’ blood and urine, including industrial compounds, pollutants, insecticides, dioxins, and mercury. Even more worryingly the study found that the study subjects tested positive for an average of 91 of them. Chemical contamination and exposure are chronic problems globally and chemical exposure has been observed as a trigger in some autoimmune conditions. A recent article on the subject noted that:
Trichloroethylene, for instance, is a solvent used in refrigerators that has been detected in the U.S. water supply and has been found to trigger an autoimmune response and compromise the gut microbiome. Mercury has been found to trigger lupus, and certain pesticides have been found to cause lupus and rheumatoid arthritis.
The Microbiome and Hygiene Hypothesis
But chemical exposure alone doesn’t seem to predict the rise in autoimmune conditions. For example, In the late 1990s, Dr. Erika Von Mutius, a health researcher, compared the rates of allergies and asthma in East and West Germany. Dr. Mutius ahead of the study anticipated that children growing up in the poorer, dirtier and less healthy East Germany would suffer from higher rates of allergy and asthma thanks in large part to the higher rates of chemical exposure they faces. What she found was the opposite. Children in East Germany had fewer allergic reactions and cases of asthma than children in the “richer and healthier” West Germany.

This leads to one of the final theorized causes of the rapid rise in autoimmune conditions, the so called “hygiene hypothesis.” The hygiene hypothesis was first introduced in the 1980s by David P. Strachan, a professor of epidemiology. He noticed that the decreasing rates of infectious diseases in a country was correlated with rises in autoimmune diseases. The hygiene hypothesis rests on the simple idea that to build a strong immune system children need early and frequent exposure to a wide variety of bacteria.
The average human body includes over 100 trillion microbes (bacteria) and this “microbiome” plays a critical role in the function of our body. Microbes stimulate the immune system, break down potentially toxic food compounds, and synthesize certain vitamins and amino acids. According to the hygiene hypothesis our microbiome is being directly affected by the nature of modern life and our lifestyle. Indeed, the microbiome of a person is highly dependent on a range of variables including diet and location. The limited dietary fiber consumption of the modern diet has been shown to cause beneficial strains of bacteria to disappear from the microbiome.
The hygiene hypothesis argues that disruptions to the microbiome are provoking the immune system of some individuals to attack healthy cells thus resulting in autoimmune conditions. The overly sanitized environments and food supply-chain as well as antibiotics in the developed world are pointed to as culprits in limiting childhood exposure to bacteria and therefore increasing rates of allergies and autoimmune conditions. Indeed, the combination of these has been shown to reduce the diversity in our gut bacteria (“the microbiome”) by up to 30%.
Overall, there is a quiet public health crisis brewing. The steep rise in autoimmune conditions is not getting the attention it deserves. More research is needed in the common causes and nature of these diseases. But more importantly, a broad debate needs to be opened in society about the role of chemicals in our food supply-chain and household products and the effect our lifestyle and dietary changes are having on our microbiome. While the science of the microbiome is early, it is clear it plays a critical role in our health and changes in the microbiome are being linked to a range of worsening public health, including the rise of autoimmune conditions.